Helping your older population when a disaster strikes
Upcoming Events
Related News
Key Takeaways
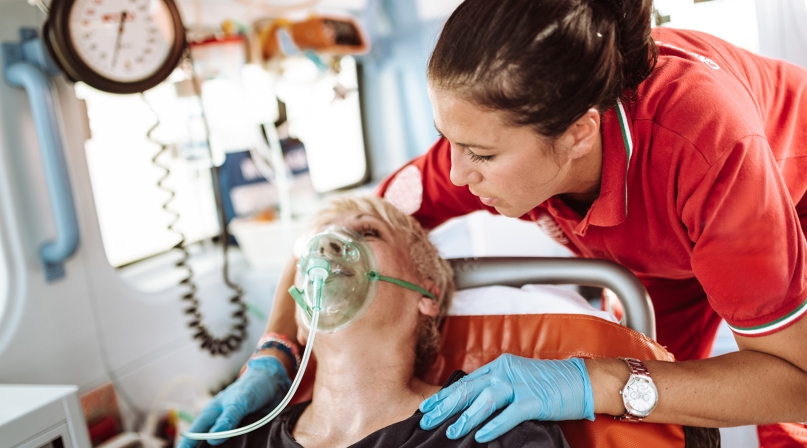
In this Q&A with Nick Boukas, preparedness director at the National Association of County and City Health Officials, he describes the particular vulnerability of older adults and people with disabilities during disasters like California’s Camp Fire tragedy and how county health departments can work to protect them.
Q. Are older adults and people with disabilities really more vulnerable during nature disasters than other populations? If so, what factors make them more at risk?
Older adults and people with access and functional needs are more vulnerable as they may require medical attention or assistance that can make evacuation more difficult. Some older adults use oxygen equipment or other medical devices, which may limit their ability to quickly leave when an evacuation order is issued. Likewise, many people, not just older adults, are on prescription medications and may not have included them in their evacuation kits along with important papers and other items needed for relocation.
NACCHO has been one of the many organizations that supports the “whole community” approach to preparedness, in which disaster planners incorporate feedback from many different stakeholders to ensure that their plans are well-rounded and inclusive. This often includes early warnings to those populations, including older adults with medical needs, to allow for additional evacuation times as well as specific instructions to ensure their safety.
Q. Do most local health departments have an emergency plan that includes these unique populations?
Local public health departments work to have processes in place to protect everyone in the community during natural disasters including older Americas, and persons with disabilities, as well as children with special health care needs, youth, pregnant and nursing moms and adults.
According to NACCHO’s 2018 Preparedness Profile (https://bit.ly/2FZeCgA) 95 percent of local health departments surveyed reported that they had incorporated the needs of older adults into their plans. We also found that 92 percent of local health departments have plans that include people with disabilities, and 87 percent have plans specific to children. Many times, this includes planning for their needs should they require emergency sheltering. Local health departments frequently work with their partners in emergency management to ensure services like dialysis and non-emergency care can still be provided to those individuals who have been displaced to a shelter until they can return home. Seventy-five percent of local health departments participate in healthcare coalitions that are made up of regional partners and stakeholders, like emergency management and Emergency Medical Services (EMS), who collaborate to work more effectively in a public health emergency. This has helped to ensure the “whole community” approach and build partnerships.
Q. What do local health departments do to protect the older adult population?
While many local health departments do not provide direct patient care, they often serve a key convening role as a coordinating body to ensure all community members are included in the response. Local health departments also staff evacuation centers and help to coordinate the needs of evacuees that may not be available at the shelter. For instance, minor wound care may be taken care of at a shelter, but those individuals who need dialysis or are reliant on medication infusions may require an advocate to work with community partners to get them their care rather than sending them to the emergency department, which can tie up those resources.
In some communities, local health departments have worked to bring long-term and assisted care facilities into their coalitions to include them in their planning. It is recommended that when considering a nursing home or assisted living facility, you should ask about their emergency plan and how they train and practice these plans.
Q. What other organizations typically partner with local health departments during emergencies?
Healthcare coalitions are made up of four key partners: local public health, emergency management, healthcare facilities and EMS. As part of the Centers for Medicare & Medicaid Services Emergency Preparedness Rule, more community stakeholders are being instructed to participate in these meetings.
Many healthcare coalitions now include long-term care facilities, dialysis centers, blood banks, public utilities, and many others that may be specific to the community. In the NACCHO Preparedness Survey, we found that more than 40 percent of local health departments offer training and assistance for their partners about how to include older adults, persons with disabilities, and children in their emergency plans.
Q. How are these emergency plans funded?
The federal government has provided some dedicated funding to help address preparedness planning at the local level since 2002 through the Centers for Disease Control and Prevention’s (CDC) Public Health Emergency Program grants.
The amount of funding, and its corresponding reach, has varied over time and are not guaranteed. Unfortunately, this program has been reduced over the years, which has a direct impact on what local health departments can accomplish.
In 2006, PHEP was included in the Pandemic All Hazards Preparedness Act, and it continues to be authorized through that law, which is past due for reauthorization. The Pandemic and All-Hazard Preparedness and Advancing Innovation Act stalled in Congress last year despite having wide bipartisan support. Efforts are already underway to get the law reauthorized this year.
NACCHO continues to work in coalition with public health, industry, and healthcare partners to get these critical programs reauthorized quickly and fully funded.
Q. What resources are available for older adults?
While important for older Americans and persons with disabilities, everyone should take the time to make an emergency kit that includes their prescription medications as well as a list with the names and dosages, important documents like insurance cards, and emergency contact information. If you have specific health care needs, we also recommend contacting your local health department to ensure your emergency needs can be met at a shelter should the need arise.
NACCHO is completing a toolkit for including Aging and Disability Networks in emergency planning. The toolkit, which will be released soon, will have information for local government offices, emergency, and community advocates on how they can best engage the different stakeholders and populations to ensure that they are considered in planning and responses. NACCHO has also developed checklists and other guides for local health departments to help inform local preparedness, which are available at http://nacchopreparedness.org/. In addition, many communities have resource centers that can provide materials for older adults and persons with disabilities. Among them are Aging and Disability Resource Centers and Area Agencies on Aging — both of these programs are under the federal Administration for Community Living.
The CDC also has a number of materials for older adults, persons with disabilities, and children and youth with special health care needs. They have recommendations on creating plans and emergency supply kits.
Many people often assume they will have time to grab items at the last minute, but frequently do not have all of their medications or prescription glasses or their medical insurance cards.
Attachments
Related News

FEMA Announces Funding Opportunity to Help Mitigate the Impact of Disasters
On March 25, the Federal Emergency Management Agency (FEMA) announced $1 billion in funding through the Building Resilient Infrastructure and Communities (BRIC) program to support disaster mitigation and recovery efforts.

DHS funding set to lapse, putting key county partners at risk of a partial shutdown
The U.S. Department of Homeland Security (DHS) is headed toward a funding lapse at 12:01 a.m. ET on Feb. 14 after the Senate failed this week to advance legislation to fund DHS for the remainder of Fiscal year (FY) 2026.
